Midline catheters and peripherally inserted central catheters (PICC) are both vascular access devices (VAD) used for infusion therapies. However, the uses of both devices are quite different.
Quiz Your Nursing Fundamentals Knowledge Here
In this article, we’ll discuss the similarities and differences of midline catheters and PICCs.
Additionally, we’ll look into:
- indications, advantages, and contraindications of both midline catheter and PICCs
- medications that should not be administered via midline catheter
- care, management, and removal of both devices
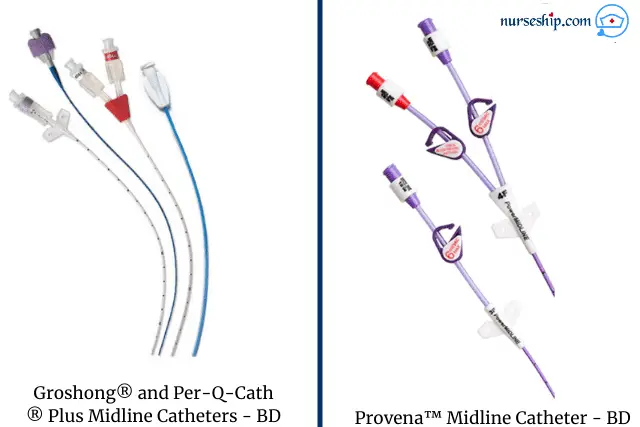
Midline Catheter
According to Infusion Nurses Society, midline catheter is defined as a vascular access device which is inserted into a peripheral vein (namely, basilic, cephalic, or brachial vein), and the tip of it is at or near axilla level, and distal to the shoulder.
The midline catheters can remain in-situ up to 30 days.
How to choose the appropriate size of midline catheter?
To choose appropriate size, estimate the distance between the axilla and the insertion site.
The length of the midline catheter ranges from 10 to 20cm, and it can have a single lumen or double lumen.
Challenge Yourself With Our Quizzes
What are the indication for midline catheter insertion?
Use of midline catheters are indicated when a patient requires intravenous therapies and blood sampling for about 2 to 4 weeks.
Other uses of midline catheters include:
- Difficult peripheral venous access
- Frequent phlebotomy
- Limited venous access on admission
- Steroids
- Fluid restricted patients
- IV drug abuse
- Diabetic patients
- Receiving multiple drugs
- Multiple hospital admissions
- Obese patients
What are the advantages of mIdline catheter?
- Use for alternate infusion therapy
- Reduce repeated venipunctures which would compromise venous access
- Can be used for 2-4 weeks
- Infusion of antibiotics, hydration, and pain medication
- Venous sampling
What are the contraindications of midline catheter?
- History of venous thrombosis
- Restricted blood flow to the extremities
- End-stage renal disease that requires peripheral vein preservation
- Known or suspected infection, bacteremia, or septicemia related to the device
- Known or suspected allergies
Medications that CANNOT be administered via midline catheters
- Continuous vesicant infusions
- Total Parenteral Nutrition (TPN)
- Chemotherapy
- Solutions greater than 600 mOsm/L
- Infusions that requires central line-only administration
- Dextrose concentration ≥10%
List of common drugs that should be avoided in midline catheters
| Acyclovir | Fosphenytoin* | Phenobarbital |
| Amiodarone | Ganciclovir | Phenylephrine |
| Amphotericin B* | Gentamicin* | Phenytoin |
| Ampicillin/sulbactam* | Iron dextran* | Potassium chloride (≥40 mEq) |
| Azithromycin* | Levofloxacin* | Promethazine |
| Calcium chloride | Mannitol ≥20% | Protein solutions >5% |
| Calcium gluconate | Meropenem* | Sodium bicarbonate |
| Caspofungin* | Morphine sulfate* | Sodium chloride ≥3% |
| Contrast media – nonionic* | Nafcillin* | Sulfamethoxazole/Trimethoprim* |
| Dexrazoxane* | Norepinephrine | Tobramycin* |
| Dextrose concentration ≥10% | Oxacillin* | TPN, exceeding 600mOsm/L |
| Dobutamine | Pamidronate* | Vancomycin* |
| Epinephrine | Pentamidine | Vasopressin |
| Foscarnet* | Pentobarbital | Zidovudine* |
*may be ok with short courses of therapy (not to exceed 3 days) with close monitoring.
ALSO, this is NOT an exhaustive list. Just examples of common medications that should not be administered via midline catheters. For specific drugs not found on this list, refer to medication package inserts or contact the pharmacy. Source
What are the complications of midline catheter?
- Infiltration
- Phlebitis
- Catheter dislodgement
- Peripheral thrombosis
- Pain
- Ecchymosis
- Edema
- Leaking
Insertion related midline catheter complications are:
- Accidental arterial puncture during insertion
- Unsuccessful procedure
- Hematoma
- Symptomatic deep vein thrombosis
Peripherally inserted central catheters (PICCs)
As the name stated, peripherally inserted central catheters (PICCs) are peripherally accessed central lines which are used for long term intravenous therapies and blood sampling.
Indications for peripherally inserted central catheters (PICC)
- Certain therapies require a central line, such as TPN and chemotherapies.
- Irritant therapies that over time can cause chemical phlebitis such as Vancomycin and Nafcillin
- Therapies lasting longer than 4 weeks
- Frequent phlebotomy
Other uses of PICC are the same as midline catheters.
Advantages of peripherally inserted central catheters (PICC)
- Administration of fluid, blood, medications in patients who do not have suitable veins for repeated access
- Preserves the peripheral veins
- Reduces the risk of phlebitis
- Decreases the risk of infiltration
- Improves comfort
- Reduces stress and pain associated with multiple venipunctures
- Eliminate complications, such as pneumothorax and great vessel perforation associated with insertions in the neck and chest regions.
- Administration of chemotherapy and parenteral nutrition therapies
- Reduced risk of air embolism
- Can be used for CVP
- Lowest incidence of complications compared to other devices
Contraindications of peripherally inserted central catheters (PICC)
- History of venous thrombosis
- History of vascular surgical procedures at the prospective placement site
- Known or suspected infection, bacteremia, or septicemia related to the device
- Known or suspected allergies
- Past irradiation of the prospective insertion site
- Preexisting skin infections
- Presence of severe peripheral edema
- Local tissue factors will prevent proper device stabilization or device access
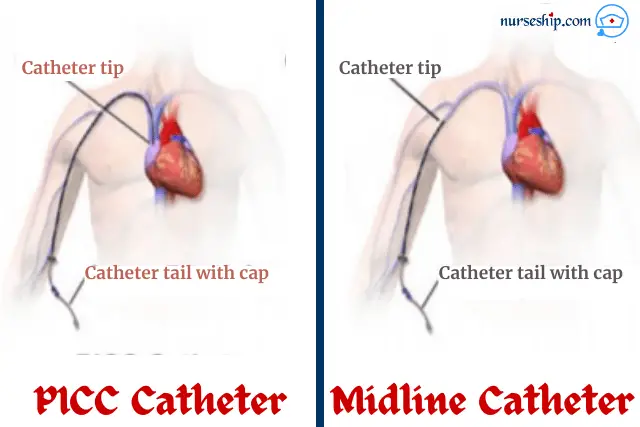
Similarities of midline catheter and peripherally inserted central catheters (PICC)
- Both are vascular access devices.
- Both can be used to draw blood samples.
- Both catheters are inserted via the same veins. Namely, cephalic, basilic, brachial, or median cubital veins in the upper arm.
- Both procedures must be performed using aseptic techniques with maximal sterile barrier precautions.
Differences between midline catheter and peripherally inserted central catheters (PICC)
| Midline Catheter | Peripherally Inserted Central Catheters (PICC) |
|---|---|
| Peripheral line | Central line |
| Catheter tip is at or near axilla level and distal to the shoulder | Catheter tip is located in the lower segment of the superior vena cava |
| Used when intravenous therapies required for less than 30 days | Used when longer lengths of intravenous therapy are needed |
| CANNOT administer certain medications (Refer to Table 1) | Can administer all types of medications |
| Radiologic confirmation is not needed before use | Chest x-ray is needed to confirm placement, unless tip locator technology is used during insertion |
| Catheter length is shorter | Catheter length is longer |
| Can’t measure CVP | CVP can be measured |
Midline Catheter and PICC Care and Management
- Flush with 5cc NS before and after routine IV/medications
- Flush with 10cc NS before and after blood draws
- Flush with 10cc NS before and after TPN (PICC only)
- Flush with 20cc NS after administering blood products
- Heparin lock and flush if no continuous infusion and not used daily
- Initially change dressing 24 hours after insertion
- Then every 7 days (use an antibacterial and antimicrobial agent to clean as per the institute’s guideline)
- Change cap every 7 days or whenever removed
- Blood pressure cuffs or tourniquets should not be used on the arm where a midline catheter has been placed
- Make sure to infuse the right and compatible drugs via midline catheter
Midline Catheter and PICC Removal
- Explain the procedure to the patient
- Gather supplies
- Remove dressing
- Gently pull out the line from arm
- Apply pressure to site
- Cover with gauze and apply occlusive dressing
- Final measurement of removed catheter
- Document the procedure
Take Our Nursing Fundamentals Quiz Here – Assess Your Knowledge
Bonus Tips
Method to choose best site for midline catheters
- Basilic vein is usually the best vein because it’s large and far from the brachial artery.
- The basilic and brachial are preferred over the cephalic vein because their higher flow ensures lower complication rates.
- Avoid the cephalic vein because its flow rate is usually lower, and gets narrower proximally.
- Avoid the cubital fossa as this site is associated with higher infection and thrombosis rates due to friction with movement.
- The ideal insertion site is proximal enough to the elbow to ensure easy elbow flexion distal enough form the axilla to ensure a 8 or 12cm midline will not cross the axilla
- Release the tourniquet until the sterile set up on the chosen arm is undertaken
Factor that needs to take into consideration when selecting a VAD include:
- Patient’s diagnosis
- Duration of the therapy
- Type of infusion
- Cognitive and intellectual level of the patient or caregiver
Check out these sample scenario-based Nursing Care Plans
3 Sample Nursing Care Plan for Hypoglycemia |NANDA nursing diagnoses |Interventions |Rationales
3 Sample Nursing Care Plans for UTI |NANDA nursing diagnoses |Interventions |Rationales
Sample Nursing Care Plan for Preeclampsia |scenario|NCP with rationales
3 Sample Nursing Care Plan for CHF [Congestive Heart Failure] (with rationales and case scenario)
3 Sample AFib Nursing Care Plans |NANDA Nursing Diagnosis |Interventions with Rationales
Sample Nursing Care Plan for Meningitis| nursing diagnosis |nursing interventions
3 Sample Nursing Care Plan for Anemia |NANDA Nursing Diagnosis |Interventions with rationales
Pneumothorax Nursing Care Plan |Nursing Diagnosis |Nursing Interventions




